
RESEARCH HIGHLIGHT: Could a new target help treat bone cancer in dogs?
Dogs diagnosed with appendicular osteosarcoma, a highly malignant and often fatal bone cancer, have limited treatment options. Current approaches have seen little success in improving outcomes, with 90% of affected dogs succumbing to the disease.
The discovery of crucial elements involved in how this type of cancer spreads (metastasizes) may hold the key to developing effective therapies for managing this extremely aggressive cancer.
In humans, Urokinase plasminogen activator (uPA) and its receptor uPAR have been linked to the spread and growth of cancer. While extensively studied in human tumours, its role in canine osteosarcoma has remained a critical knowledge gap. Given the aggressive nature of canine osteosarcoma and the success of the uPA system as a novel marker in human cancers, first author, graduate student Dr Arata Matsuyama (DVSC), and a team of OVC researchers set to explore the significance the urokinase plasminogen system in dogs with appendicular osteosarcoma.
Their study involved a comprehensive analysis of serum and tissue uPA/uPAR expression in dogs diagnosed with osteosarcoma. The results were promising; dogs with osteosarcoma had significantly higher levels of uPA in their blood than healthy dogs (median 1905 vs 1440 pg/ml, p = 0.008). Moreover, a majority of canine osteosarcoma cases showed uPA (75.9%) or its receptor, uPAR (77.6%), or both (70.1%) in their tissue samples, indicating a potential influence on disease progression.
The findings suggest that the uPA system could serve as a diagnostic marker for canine osteosarcoma, offering a less invasive method for testing. The high prevalence of uPA and uPAR expression in tissue samples indicates that the urokinase plasminogen system may play a significant role in the tumour’s microenvironment, possibly influencing disease progression. However, further research is needed to confirm its prognostic significance and explore the potential of uPA and uPAR as targets for therapeutic intervention in dogs with osteosarcoma.
The full publication can be found here: Prognostic significance of the urokinase plasminogen activator system in tissue and serum of dogs with appendicular osteosarcoma – Matsuyama et al, 2022

RESEARCH HIGHLIGHT: Can new information about feline heart disease also help humans? What is the significance of microRNA?
Hypertrophic cardiomyopathy (HCM) is a common heart disease in humans and cats, however, we don’t really understand how this disease develops. In cats, HCM is characterized by excessive thickening of the heart muscle, particularly the left ventricle (LV). This thickening results in abnormal diastolic function, heart failure and in many cases sudden death. Interestingly, HCM in humans is remarkably similair to cats in terms of its behaviour, symptoms, and histological (or tissue) changes.
Previously, our cardiology research team led by Dr. Sonja Fonfara has shown that cats are an excellent translational model for understanding human HCM. This has been expanded upon in recently published research by first author, graduate student Jessica Joshua (PhD) in collaboration with researchers at the University of Zurich and Prince Edward Island.
MicroRNAs (miRNAs) are small non-coding regions of ribonucleic acid (RNA), which help to control the type and amount of proteins that a cell makes. This is important as it impacts the expression of genes and downstream cellular and metabolic pathways. Abnormal expression of miRNAs has been linked to various diseases including HCM. Using RNA sequencing technology, the team was able to profile over 1000 differentially expressed microRNAs in the hearts of healthy cats and cats with HCM. Eighty miRNAs in the left ventricle and 37 in the left atrium were characterized.
Cats with HCM were found to have a distinct miRNA expression profile with regional differences within their hearts. These included enriched miR-21, miR-146b and reduced miR-122-5p; all miRNA which have been recently suggested as central to HCM development in humans. Also enriched was miR-132 which could be of therapeutic interest. Interestingly, they also found that the genes regulated by these miRNAs are involved in early and late-stage development pathways of HCM.
Going forward, this project can serve as a template for future studies seeking to understand the causes and mechanisms of HCM in cats and humans.
The full publication can be found here: MicroRNA profiling of the feline left heart identifies chamber-specific expression signatures in health and in advanced hypertrophic cardiomyopathy
The previous article about cats as a translational model can be found here: Feline myocardial transcriptome in health and in hypertrophic cardiomyopathy—A translational animal model for human disease | PLOS ONE

RESEARCH HIGHLIGHT: Can new immunotherapies that have shown promise for humans also be used to treat our pets?
Urothelial carcinoma (UC) is the most common urinary bladder tumour in dogs, but little has advanced in the way we treat this disease. While there is a range of therapeutic options including surgery, chemotherapy, and radiation therapy, the prognosis has only slightly improved.
In humans, muscle-invasive urothelial carcinoma (MIUC) looks and acts very similar to what we see in dogs and because of this, UC has the potential to be an excellent translational disease model. Innovations in immunotherapy using novel checkpoint inhibitor therapies have greatly expanded options and shown promise for people diagnosed with MIUC, especially when the disease is non-resectable (via surgery) or has metastasized.
Graduate students Dr Christopher Pinard (DVSc) and Ashley Stegelmeier (PhD), compared the level of lymphocyte-specific PD-1 and cytokine expression in the blood and urine of canine UC patients to healthy control dogs and dogs with cystitis (urinary infections). PD-1 is a crucial protein of the immune checkpoint blockade, an important biomarker, and has the potential to be a determining step for immunotherapies. Cytokines are chemical compounds released by many types of cells and influence the body and tumour microenvironment.
Cytotoxic T-cells in the urine had significantly higher PD-1 expression when compared to healthy dogs. T-regulatory cells, important cells that can suppress the immune response were also elevated in UC and cystitis patients. There were also elevated cytokines in the urine correlated with high PD-1 or PD-L1 expression.
Interestingly, the result from this study mirrors the data found in previous human studies of MIUC. Given the success of immunotherapies in human MIUC, and the evident immune-based similarities between species, this suggests that immunotherapies may also be an effective strategy to treat the disease in dogs.
The full publication can be found here: Evaluation of lymphocyte‐specific programmed cell death protein 1 receptor expression and cytokines in blood and urine in canine urothelial carcinoma patients – Pinard – 2022 – Veterinary and Comparative Oncology – Wiley Online Library
RESEARCH HIGHLIGHT: Seizures are underreported in human medicine – is this also true for dogs with epilepsy?
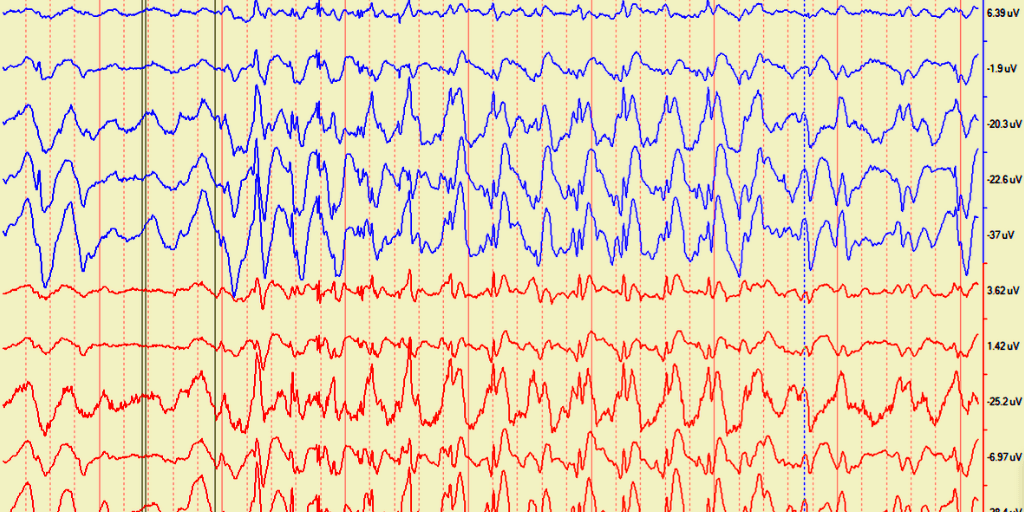
Caregiver or patient descriptions are regularly used in both human and veterinary medicine to diagnose seizures. This is known as ‘subjective data.’ On average, human patients document fewer than 50% of their seizures. This underreporting is why electroencephalography (EEG) testing is fairly standard. Via small electrodes placed in/on the scalp, an EEG is the only real-time routine detector of the abnormalities in the electrical activity of the brain that are called seizures. An EEG is a measure of ‘objective data.’
First author, graduate student Dr Masayasu Ukai (MSc), wanted to explore if the seizure underreporting phenomenon also exists in veterinary epileptology. This was a collaborative study amongst five academic and private veterinary referral hospitals, with 33 dogs meeting the study criteria. The number of seizures based on epileptogenic paroxysmal discharges (PDs) on the EEG was compared to the reported seizure frequency described by each dog’s caregiver. There was only a weak correlation (0.39 (95% confidence interval [CI]=0.048-0.64,P=.03)) found between seizure frequency reported by caregivers (subjective) and the actual seizure frequency on the dogs’ EEGs (objective).
While more research is needed, these findings suggest that seizure underreporting also occurs in veterinary medicine. To provide the most accurate diagnosis, EEGs in dogs should be performed to determine seizure frequency, especially when dogs are suspected to manifest myoclonic seizures or behavioral arrest (absences). This is aligned with the International Veterinary Epilepsy Task Force recommendation to use EEG data to increase the accuracy of seizure reporting and diagnosis.
Funding for this research was generously provided by OVC Pet Trust. The full publication can be found here: Seizure frequency discrepancy between subjective and objective ictal electroencephalography data in dogs – Ukai – 2021 – Journal of Veterinary Internal Medicine – Wiley Online Library

RESEARCH HIGHLIGHT: An innovative “seek and destroy” alternative to cancer surgery for people and pets is being tested for the first time this year at the University of Guelph’s Ontario Veterinary College (OVC).
During the trial, researchers aim to refine the novel nanomedicine treatment (Porphysomes) for use in animals and, ultimately, this therapy will be used for treating various types of human cancer as an adjunct or alternative to surgery. The U of G team with Research Chair in Veterinary Medical Innovation, Dr Michelle Oblak (Veterinary Innovation (uoguelph.ca)) is working with UHN researchers, including head and neck surgeon Dr. Jonathan Irish and Dr. Gang Zheng, the inventor of this technology.
Dr Oblak and her team injects the porphysomes into the bloodstream; these nanoparticles collect in the tumour or any spot where the cancer may have spread. The light-activated molecule’s fluorescent glow allows the team to track its location using a special light source. Besides pinpointing the tumour’s whereabouts, the porphysomes make the tissue more vulnerable to damage from laser light. A beam of near-infrared laser light directed through a nano-fibre activates the porphysome, which then destroys cancerous tissue. For the clinical trial, the team is destroying only a portion of the tumour, then taking samples of the tumour and lymph nodes to assess results of the therapy. Patients in the trial still undergo standard-of-care surgery to remove the entire tumour.
More information on this study can be found on our actively recruiting studies page (Canine Clinical Trials With Active Recruitment – OVC Clinical Trials (uoguelph.ca)) and the full news release(s) are linked here: can be found here: OVC Researchers Test ‘Seek and Destroy’ Cancer Treatment – U of G News (uoguelph.ca) and OVC Researchers Test ‘Seek and Destroy’ Cancer Treatment | Ontario Veterinary College (uoguelph.ca) and Ontario Veterinary College researchers test ‘seek and destroy’ cancer treatment (uhn.ca)
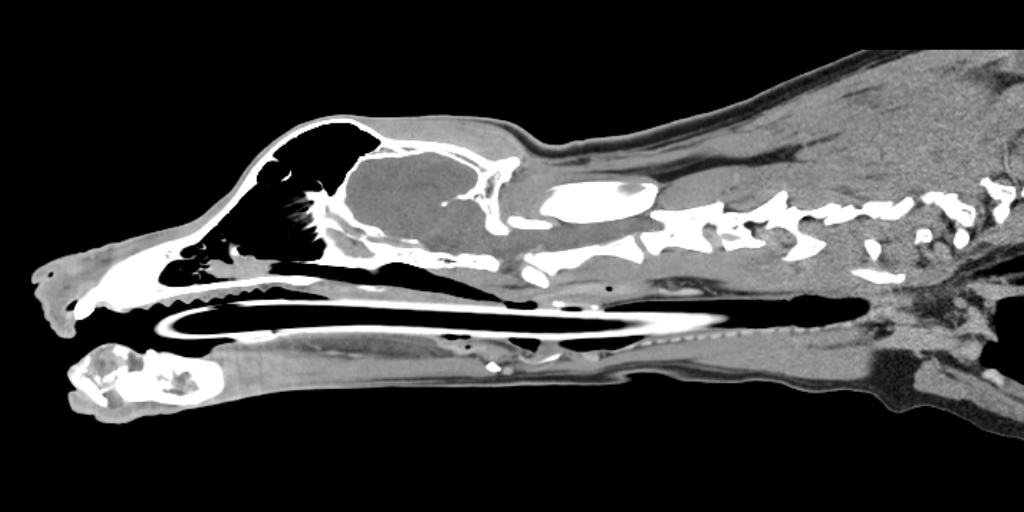
RESEARCH HIGHLIGHT: Should a combination of preoperative and intraoperative modalities be used for disease evaluation in dogs with oral tumours?
In veterinary oncology, understanding the spread of disease to lymph nodes is extremely important. In dogs with oral tumours, lymph nodes that are surrounding the oral cavity are most often affected but which lymph node the tumour drains to can be variable. Sentinel lymph node (SLN) mapping helps us to better understand how these tumours drain and ensures the correct lymph nodes(s) are sampled. There are a couple ways to approach SLN mapping, we can perform a specialized computed tomography lymphography (CTL) before surgery or during surgery, we can use a fluorescent dye, Indocyanine green (ICG) with specialized near infra red fluorescence (NIRF) camera and/or methylene blue (MB) dye.
First author, graduate student Dr Jen Wan (DVSc), used both CTL and ICG NIRF +/- MB lymphography (IOL) in 14 client-owned dogs with oral tumours. In these 14 patients, a total of 57 SLNs were identified. When CTL and IOL were combined, the overall SLN identification rate was 100%. ICG NIRF identified a greater proportion of SLNs (91%; 52/57) compared with MB (50.8%; 29/57) and CTL (42.1%; 24/57).
This research confirms that both preoperative and intraoperative techniques for SLN mapping are simple and feasible to perform. The combination (CTL and IOL) may greatly improve the ability to accurately detect the SLN in dogs with oral tumours.
Funding for this research was generously provided by OVC Pet Trust. The full publication can be found here: Determining agreement between preoperative computed tomography lymphography and indocyanine green near infrared fluorescence intraoperative imaging for sentinel lymph node mapping in dogs with oral tumours – Wan – 2021 – Veterinary and Comparative Oncology – Wiley Online Library

RESEARCH HIGHLIGHT: Can a dog’s own immune system be used to treat bladder cancer?
Urothelial carcinoma (UC) is the most common urinary tumor in dogs and it behaves, looks, and genetically appears to be similar to muscle-invasive urothelial carcinoma (MIUC) in people. This makes UC in dogs an excellent model for the disease in humans! In humans, the use of immunotherapy (using the patient’s own immune system to target the cancer) has shown promise as a therapy for patients with MIUC and is being incorporated into the standard-of-care.
Immune checkpoint molecules are a normal part of the immune system and help to ensure that our immune response is not sent into overdrive against our own normal cells. Some cancers will take advantage of this system to “turn off” the immune system against themselves, allowing the tumour to continue to grow… think of putting your foot on the brakes of a car. By using immunotherapies that lift your foot off the brakes, we effectively turn the immune system back against the cancer cells and can lead to better outcomes in cancer patients.
The programmed death ligand-1 (PD-L1) and its receptor, programmed death receptor 1 (PD-1) is a well-described immune checkpoint in several human cancers, including UC and MIUC. Typically, the receptor (PD-1) is housed on immune cells, and PD-L1 resides on other cells (cancer cells, stromal cells).
First author, graduate student Dr Christopher Pinard (DVSc) with assistance from members of Drs Hocker and Mutsaers research teams, evaluated the expression of PD-L1 and PD-1 in canine UC cell lines via flow cytometry, western blot analysis, reverse transcription PCR (RT-PCR) and fluorescence microscopy. Excitingly, this study provides the first evidence of cell-intrinsic PD-1 expression in canine UC. The team also demonstrated that canine UC cell lines have protein and gene expression of PD-1 and PD-L1, meaning that these immune checkpoints could be attractive targets for immunotherapy for the treatment of UC in dogs.
The full publication can be found here: Evaluation of PD-1 and PD-L1 expression in canine urothelial carcinoma cell lines – ScienceDirect
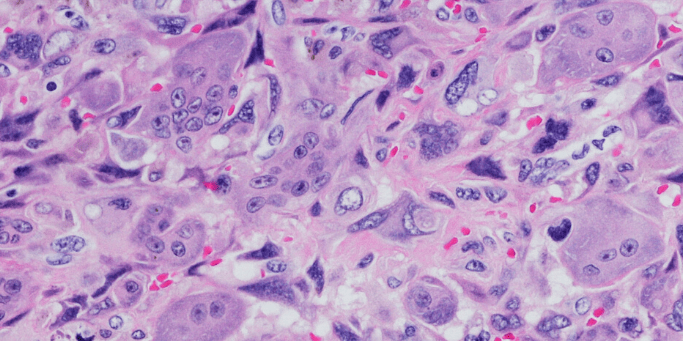
RESEARCH HIGHLIGHT: Second opinion histopathology – should it be used in veterinary medicine?
In human medicine, it’s common practice to have surgically-removed tissues reviewed histologically (under a microscope) by more than one pathologist (whose area of expertise is body tissues and body fluids) before pursuing cancer treatment. This second opinion is used to confirm the original diagnosis or identify discrepancies, which could alter the course of disease, cost of treatment, patient management or prognosis.
First author, graduate student Dr Sarah Laliberte (DVSc), retrospectively explored the major factors which influence the decision to pursue a second opinion histopathology in veterinary oncology patients and when used, if there was disagreement between the opinions. Most commonly, a second opinion was sought when the tumour was either atypical/poorly differentiated (31%) or the results of a biopsy did not fit with the symptoms and signs of the disease in the pet (25%). Major disagreement (a change in diagnosis between both opinions, that resulted in the alteration of treatment recommendations) occurred in 39% of cases. While second opinion may not be routinely practiced in veterinary medicine, it could have a beneficial role to optimize disease therapy and better predict patient outcomes.
The full publication can be found here: A retrospective comparison of first and second opinion histopathology with patient outcomes in veterinary oncology cases (2011–2019) – Laliberté – 2022 – Veterinary and Comparative Oncology – Wiley Online Library

RESEARCH HIGHLIGHT: Are you a Cat Whisperer?
Cats are notoriously mysterious with moods and expressions that are difficult to decipher. Inspired by their own pets, researchers Drs. Georgia Mason and Lee Niel conducted an online survey to explore how well we can judge the facial expressions of cats.
Out of thousands of participants, only 13% received an excellent score, accurately identifying ‘positive’ and ‘negative’ expressions. Women, young millennials or veterinary professional were more likely to score higher. This study may allow for the development of tools that would help both veterinary professionals and pet owners better understand their feline friends!
Read the full story about this research on the OVC Pet Trust site: Am I A Cat Whisperer? | OVC Pet Trust (uoguelph.ca) and find out how you’d score in the survey: http://uoguel.ph/catfacequiz


